Surgical Procedures List
Mr Edwards maintains expertise in the following areas:
Bunions (Hallux Valgus) are caused by instability of the joint at the base of the big toe and by miss-shaped bone here. If there is instability, deformity will progress with time.
Often bunions cause pain for a variety of reasons including the prominence rubbing on shoes; degenerative change (arthritis) and inflammation as joint structures are stretched. Decreased function of the big toe puts more stress on the remainder of the forefoot resulting in lesser toe problems including corns, claw toes, and occasionally, ulceration or infection.
Not all bunions are problematic – in most cases surgical treatment is optional.
Non surgical treatment involves the modification of shoes so that there is enough room to fit the foot in the shoe without tightness. Typically a shoe with a fairly solid sole is needed. Insoles may lessen pain in outer aspect of the foot but rarely slow the progression of bunion deformity. Sometimes anti-inflammatory drugs help.
Why it can get worse
Progression is driven by unbalanced muscle pull with a weak joint. Because the muscle pulls hard with every step is pretty much impossible to stop things getting worse without surgery once the toe position really starts to move.
Surgery Choices
There are very many different surgeries for bunions; the choice of surgery will depend how big it is and how much arthritis is in the joint. Better surgeries are those that rebuild a normal joint giving good position, shoe fit and movement. It involves cutting the bones to put them in a good position without damaging the cartilage and then balancing strength at the joint (moving tendons or muscles, tightening ligaments so that pull is even).
If the joint is very arthritic then the fall-back option is to fuse it – this is counter-intuitively successful surgery but is confined for those whose toes are stiff and very painful. It leaves a very high level of activity but will stop you from wearing high heeled shoes.
Surgery is performed in hospital as an inpatient or day surgery. Usually you can walk on the foot on the day of the surgery, but for the first week or two, most of your time is spent in bed to let the skin heal.
After that, activity increases although the bones will not solidify for around two months and be really sound by four months.


Claw, Hammer and Mallet toes all involve a degree of contracture (stiffness and “deformity”) of the joints of the involved toe.
The cause is not always clear. It may result from dysfunction of the small muscles of the foot, an associated deformity of the great toe (eg crowding with bunion deformity), by forcing the toes into shoes which are too small, trauma or hereditary factors.
The joints involved become prominent and rub. Friction between the shoe and a bony prominence causes the skin to thicken and form a corn or a callosity (occasionally even an ulcer) on the top of the toe or at its tip. The corn, not the deformity, is often the most troublesome problem.
Occasionally the affected toe under- or over-lies its partner.
Sometimes the bony prominences of toes simply become prominent rather than the joints being contracted. They may rub on each other or the shoe to cause a callous.
When toes rub together, the skin often macerates and causes an extremely painful (and obscure) “soft corn” or ulcer.
Operative intervention may be needed particularly if there is recurrent ulceration or infection.
Great toe deformity correction is frequently needed to reduce both crowding and stress.
Ill-fitting shoes and improper nail trimming are two of the most common causes of an ingrown toenail. Other causes include fungal infection or nail injury.
Swelling, pain, redness and sometimes infection are symptoms of an ingrown toenail.
Conservative treatment includes regular podiatry and wearing comfortable spacious shoes.
Surgical Solutions
There are a number of surgical procedures to cure an ingrown toenail which are done as day surgery .
A nail ablation is where the nail growing into the skin is cut away. This procedure is not permanent as the germinal matrix of the nail is not affected.
A wedge or partial resection will leave a cosmetic nail.
The most reliable procedure involves removing a wedge of nail and destroying the germinal matrix. This will then inhibit the cells from growing a new nail. This results in a permanently narrower nail.
3 days will be needed off work. The toe will be sore after this procedure and pain medication and oral antibiotics will be provided.
Dressings are removed on day 3 when the foot is soaked in warm, salty water and re-dressed.
Ankle fractures are common and if misdiagnosed or left untreated, they can lead to long term pain and arthritis.
There are many different types of ankle fractures. Most require surgery to realign the bones and ankle joint.
Open reduction and internal fixation (ORIF) is usually performed by installing plates and screws that secure the bones in the proper anatomical position during the healing process.
Sometimes these need to be removed at a later date after the initial surgery.

Chronic pain and instability following ankle sprain
An ankle sprain is an extremely common sporting injury. Tearing of the lateral ligaments is often accompanied by intra-articular pathology which can contribute to longstanding ankle pain and instability.
If, after rigorous physiotherapy, recurrent ankle sprains and instability is experienced, surgery for stabilisation is recommended. By ensuring the ankle ligaments are strong, this makes the ankle stable and helps prevent further injury.
Osteo Chondral Defect (OCD)
When a patient has a history of ankle instability and repeated sprains, both the bone and cartilage will be affected. Minor injuries should recover with rest and elevation.
More severe injuries may result in loose bone fragments and cartilage in the ankle joint which may result in surgery. The severity of the injury determines if surgical intervention is required.
Arthroscopy and Ankle Reconstruction
This surgery is primarily aimed at removing any materials that may promote infection and impede healing the ankle joint as well as stabilising the surrounding ligaments and preventing arthritis.
Both surgeries are done at the same time, allowing any underlying joint pathology to be treated as well as stabilising the joint.
Ankle Arthritis
Arthritis affecting the ankle joint typically presents as a painful stiff ankle. There are a variety of causes for ankle arthritis and there are a number of surgical procedures aimed at addressing symptoms.
Non surgical or conservative treatment includes: bracing, shoe wear selection, exercise and pain medication.
The type of ankle surgery will depend on the severity of the disease and the level of symptoms experienced.
Ankle Fusion
An ankle fusion is the most reliable surgical option when the ankle is stiff and painful. The degenerate joint surface is surgically removed and then fixed together with screws. The bones heal in this position and should remain in situ permanently.
This surgery aims to convert a stiff painful ankle joint into a solid comfortable joint.
Ankle Replacement
This surgery is aimed at preserving ankle joint motion. The worn out joint surfaces are removed and replaced with a metal implant that functions similarly to a normal ankle joint. Whilst this is a less reliable option than the ankle fusion, performed on a suitable patient can produce desired results.
The Achilles Tendon is located at the back of the leg and connects the calf muscle to the calcaneus. It is the thickest, strongest and longest tendon in the human body.
Acute Rupture
Playing sports is the most common reason why a Tendo Achilles rupture occurs It is most commonly reported in patients aged 30 to 40. Often patients describe hearing a pop, which is followed by sharp pain, tenderness and weakness.
Full strength is rarely fully regained without the aid of surgical intervention after an Achilles rupture. Clinical diagnosis in isolation is common but an ultrasound is a useful supporting diagnostic test.
Conservative treatment is generally not recommended for people who wish to lead an active lifestyle.
The most common treatment is surgical repair. The benefit of surgery is that maximum strength of the tendon is regained. The surgeon must ensure correct tension and length at time of surgery.
Mr Edwards has an integral role in ensuring the correct tension and length of the tendon.
After the surgery the patient is placed in a cast for approximately two weeks.
At the follow up appointment this cast is generally replaced with a CAM boot. The patient remains non weight bearing for 6-8 weeks post surgery.
After this time the patient will weight bear in the CAM boot for 2-3 weeks, then progress into a supportive shoe with a heel raise.
Rehabilitation is vital. Physiotherapy and hydrotherapy should be undertaken to facilitate recovery and explosive sport should be avoided for at least six months.
The midfoot is comprised of a number of joints called the tarsometatarsal joints.
Arthritis of the midfoot may affect one or all of these joints. It may be caused from previous injury to the joints, or from every day ‘wear and tear’.
Generally presenting as aching pain on the top (dorsum) of the foot, it can be worse with activity and shoe wear.
Non surgical treatment of midfoot arthritis includes:
shoe wear modification, insoles, pain medication and change in activity.
Midfoot Osteotomy
There may be prominent bony bosses on the top (dorsum) of your foot. If this is painful, rubbing and making shoe wear difficult, it is possible to surgically remove (osteotomise) the bony bump to negate these symptoms.
The most common operative treatment for midfoot arthritis is a fusion (arthrodesis) of the tarsometatarsal and or cuneiform joints to convert stiff painful joints into solid comfortable ones.
The degenerate joints are surgically removed and held together with plates and screws. They routinely remain in situ.
Flat Feet (pes planovalgus) is a common complaint with differing levels of severity and symptoms.
The degree of severity directly impacts the surgical decision. There are numerous other factors such as; pain,age, weight, degree of arthritis and bone density that influence the type of surgical procedure.
Conservative treatment includes insoles, supportive shoe wear, analgesics, anti-inflammatories and a change in activity.

Reconstruction
Flatfoot reconstruction is both complex and demanding and the procedure can vary according to individual requirements.
The aim of reconstruction surgery is to improve foot anatomy, function and pain. Reconstruction surgery can include numerous small osteotomies, ligament and tendon reconstructions, bone grafting or lengthening tendo Achilles.

Subtalar Fusion
If it is determined that the severity of your problem inhibits reconstructive surgery, fusion (arthrodesis) of the subtalar joint can be an option. This surgery aims to realign the hindfoot and alleviate pain.
A Subtalar fusion is used for a variety of hindfoot conditions and the type of surgery required will be determined by Mr Edwards.
Another surgical solution used to treat both troublesome flat feet and hindfoot arthritis is a procedure called a triple fusion. This is where the subtalar joint, calcaneocuboid and talonavicular joints are fused.
This surgery is aimed at making a stiff problematic foot into a strong comfortable functional one.
Plantar Fasciitis is a common condition. It causes heel pain, which may be debilitating.
Usually it is worse when standing after a period of rest – for instance when standing or arising from bed after sleep. It is also worse after walking or standing for an extended period particularly on rigid surfaces.
If left untreated, the condition typically lasts two years or more, often leaving residual discomfort. This time course often can be shortened with appropriate treatment.
Anatomy
The Plantar Fascia is in the sole of the foot & prevents the arch of the foot spreading.

From the heel to the toes of a foot there is a longitudinal arch; the plantar fascia. It is a thick cord of fibrous tissue, which bridges this arch. It is like a tie-bar – it prevents the arch from spreading just as a tie bar would in a building. Whenever there is weight put through the foot, the plantar fascia is under tension and stretched.
Pathology
Fatigue failure of the fascia causes fasciitis – “wear gets ahead of repair”.
Repeated stretching of the fascia is like bending a wire coat hanger. As the hanger is repeatedly bent, it fatigues – “becomes hot” – it eventually breaks.
In the foot a repair mechanism prevents fatigue failure. However, with age this repair mechanism can fail. In a sense, the problem in plantar fasciitis is that “wear gets ahead of repair” and “hot” inflammatory tears develop in the fascia at the heel.
Tension or repeated compression of fascia causes pain. Pain is experienced when the “hot” or inflamed and partially torn fascia is stretched from the resting or shortened state to its’ natural length (as in standing and walking after rest).
It is also caused when this inflamed or bruised area suffers recurrent pressure (such as with standing or walking for an extended time).
Nerves in close association with the fascia may be involved in the inflammatory process and contribute to the pain.
Recommended Treatment
Treatment should initially be aimed at keeping the fascia at its natural length (rather than having it repeatedly change length and hence suffer fibre disruption) and to cushion it.
The first line treatment is to stretch the fascia and keep it stretched allowing it to heal at its “natural” length.
Stretching is best done at least four times a day and must be performed every day.
Whilst standing with the balls of your feet on a step (with the knees kept straight), the heels are then gently dropped as you count to ten. Do not bounce.
Lift the heel and count to five or ten and repeat the cycle. Tightness will be felt both in the sole or heel of the foot and at the back of the leg (as the tendo-achilles is also stretched).
Cushion the Heel
A thick heel pad – typically eight to ten millimetre thick silicon (for instance a Viscospot insert) should be used to provide cushioning in the shoe and protect the heel.
If this program is used the fascia heal and condition slowly improves typically over a twelve-week period – complete healing will take at least six months.
Other options
The heel may not respond to this simple first line approach. Often the use of non-steroidal anti-inflammatory medication will assist in speeding recovery.
Alternative treatments include night splints (which keep the fascia stretched out to length overnight), steroid injection, ultrasound lithotripsy treatment or specially made insoles.
If such techniques fail, casting may be required and very occasionally, surgical release.
Surgery is rarely required
Surgical treatment involves the excision of the inflamed tissue and usually release of nerves in the heel (which are often affected in severe cases).
I do not (or at least extremely rarely) excise the bony “heel spur” often associated with this condition as it is an unusual cause of pain and its’ excision increases the risks of surgery.
Surgery is not used as a first line treatment. Although results can be excellent, there is a significant group of patients in whom it fails to improve the condition, or may even make the problem worse. Therefore, I recommend trying non-operative options first.
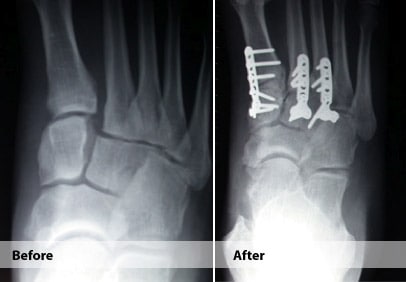
Lisfranc Injury
Lisfranc Injuries (Tarsometatarsal Injuries) are uncommon fractures or dislocations of the midfoot that typically occur during a fall or twisting motion. They can be misdiagnosed as a ‘sprain’. These injuries present with pain and swelling on the top of the foot and often bruising on the bottom of the foot.
Non-operative treatment such as plaster immobilisation is not ideal and can lead to increased risk of post traumatic midfoot arthritis.
There are a number of surgical procedures used to treat a Lisfranc fracture. Surgery allows the anatomy of the midfoot to be reconstructed. Typically these fractures are treated with inserting screws or plates.
Post op, the patient will be placed in a cast and non-weight bearing and the cast remains on for a period of 6 weeks. The patient will then be placed into a CAM boot enabling full weight bearing for a further 4-6 weeks. After this time, a solid supportive soled shoe with an insole will be worn.
Tibial Plafond fractures
There are various different methods used to treat these fractures and the type of surgery is determined on an individual basis. This fracture involves the ankle joint and can involve the joint surface. These must be treated surgically to help minimise the risk of deformity, pain and arthritis.
Calcaneal Fractures
Calcaneal fractures are commonly sustained from high impact activity such as a fall from a height or sporting injuries. The majority of these injuries require surgical intervention to reposition and realign the bone to aid in prevention of arthritis, pain and deformity.
